Breast Care During Breastfeeding Period
Your breast will change during pregnancy and during the postpartum period. Hormones released by your body during pregnancy will make your breasts grow and produce breast milk.
After the birth of your child, your breasts will start to fill up with breast milk in anticipation of feeding your hungry baby. Your breast will be larger and feel tender due to milk engorgement which may leak through the nipples. It is important to take good care of your breasts to prevent problems during breastfeeding.
Breast Care during Breastfeeding
- Practice good hygiene by washing your breast and nipples with warm water while having your bath or shower. Do not use too much soap as it may dry your nipples causing them to crack.
- Wear a supportive nursing bra which is not too tight and preferably made of cotton so that it does not sweat too much. Use breast pads to prevent milk leakage wetting the bra. This prevents fungus (thrush) growth and also makes it comfortable for you.
- Get your baby to latch correctly from the first breastfeed and breastfeed regularly (at least every 2 to 3 hours) to prevent the development of painful breast engorgement, plugged milk ducts and mastitis. If your baby does not want to feed, pump the breast milk to release the milk and encourage the breast to produce a healthy supply of milk.
- Moisturize your nipples with your breast milk after breastfeeding and then let the nipples air dry naturally.
- Remove your child from your breast correctly. When you’re ready to take your baby off the breast, do not pull him/her off but instead, place your finger in the corner of her mouth to break the suction between the mouth and your breast.
Common Breast Issues during Breastfeeding
1. Blocked Milk Ducts
Blocked milk ducts occur when you are making milk faster than it is used or there is incomplete emptying. Other causes include pressure from an ill-fitting bra, stress, previous breast surgery scar and incomplete latch. The blockage feels hard and tender to touch. Treatment options include;
- Warm compress and gentle massage towards the nipple to help express the blocked milk
- Position your baby to suck at the blocked duct area
- Have more rest to reduce stress and stay hydrated
2. Sore or Cracked Nipples
Cracked nipples are common and give rise to pain during breastfeeding. It typically arises 3-7 days postpartum and can increase the risk of nipple infection and mastitis. Cracked nipples can be treated with 100% lanolin or glycerin/hydrogel nipple pads placed over the nipples to help soothe and heal cracked or painful nipples.
3. Mastitis
Mastitis is breast inflammation (usually due to infection) and is common during the first 6 months of breastfeeding. Failing to empty the breast milk or going for long periods between feeds causes the breast to be engorged with milk.
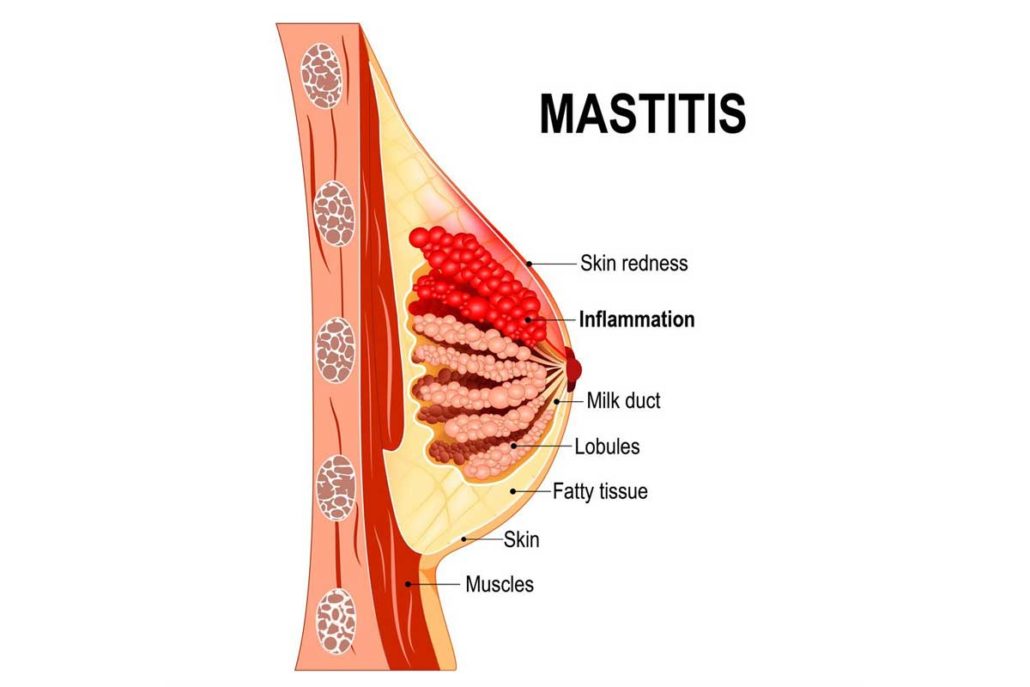
Infection happens when bacteria enter the breast through the nipple and is more common when the mother has a cracked or sore nipple. The symptoms are redness, tenderness or pain which may be accompanied by fever. Seek treatment immediately to prevent abscess formation. Mastitis is treated with antibiotics which will not harm the baby and painkillers for the pain. In the meantime, you can do the following ;
- Get more rest, drink more fluids and you can place a warm wet pack on your painful breast or massage the breast gently to increase the milk flow.
- Feed your baby with your OTHER healthy breast.
- If the nipple of the affected breast is too painful to breastfeed, use a breast pump to empty the breast of milk. This will help the mastitis get better faster.
How to maintain Continuous Milk Production to Reduce the risk of Blockage & Inflammation
- Have a healthy well-balanced diet, keep hydrated and feed (or pump) regularly (around every 2-3 hours) is the secret to maintaining a good milk supply
- Foods which encourage milk production are called lactogenic foods. Some of the examples of lactogenic foods are oatmeal, barley, green leafy vegetables, garlic and almonds
- Medications which encourage milk production are Metoclopramide and Motilium which can be used to increase milk production as a last resort.
If you have any concerns about your breasts or how to care for them during breastfeeding, do contact your Doctor, Gynaecologist, Mid-Wife or a Lactation Consultant
Disclaimer. TELEME blog posts contains general information about health conditions and treatments. It is not intended to be a substitute for professional medical advice, diagnosis or treatment. The information is not advice and should not be treated as such.
If you think you may be suffering from any medical condition, you should seek immediate medical attention from your doctor or other professional healthcare providers. You should never delay seeking medical advice, disregard medical advice, or discontinue medical treatment because of information on this website.