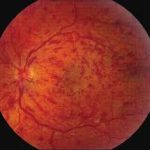
Types of Diabetic Eye Disease (Retinopathy)
Diabetic retinopathy is the most common cause of blindness in young adults and is caused by poorly controlled diabetes. It is preventable but requires the patient to take good care and good control of the diabetes condition.
Who is at risk for Diabetic Eye Disease
- Long duration diabetes (the longer you have diabetes, the greater the risk)
- Poorly controlled diabetes
- Diabetics who smoke
- Diabetics who have co-existing conditions such as hypertension, cholesterol or kidney disorder
- Pregnancy with diabetes
- Diabetics who have unhealthy lifestyle such as being overweight, do not take care of their food intake or seldom exercise
Symptoms of Diabetic Eye Disease
The symptoms are:
- Fluctuating vision or difficulty focussing
- Blurred Central or Peripheral Vision
- Sudden onset of Floaters (black spots or wavy lines floating in your field of vision)
- Sudden loss of vision in one eye
Types of Diabetic Retinopathy
There are several stages of diabetic retinopathy. Retinopathy (also known as retina damage) occurs because there is too much sugar in your blood which disturbs the delivery of nutrients and oxygen to the eye. The higher the sugar level or the longer duration of your disease, the greater risk is your retina damage.

1. Non-Proliferative Diabetic Retinopathy
Background or Non-Proliferative Diabetic Retinopathy occurs in some patients after many years of having diabetes. There will be some microaneurysms and other changes in the small blood vessels in the retina and may be accompanied by some leakage of exudates at the peripheral retina. Although this stage does not cause any eye symptoms, it is important to see your eye doctor and diabetic doctor to help you manage your diabetic control better.
2. Proliferative Diabetic Retinopathy
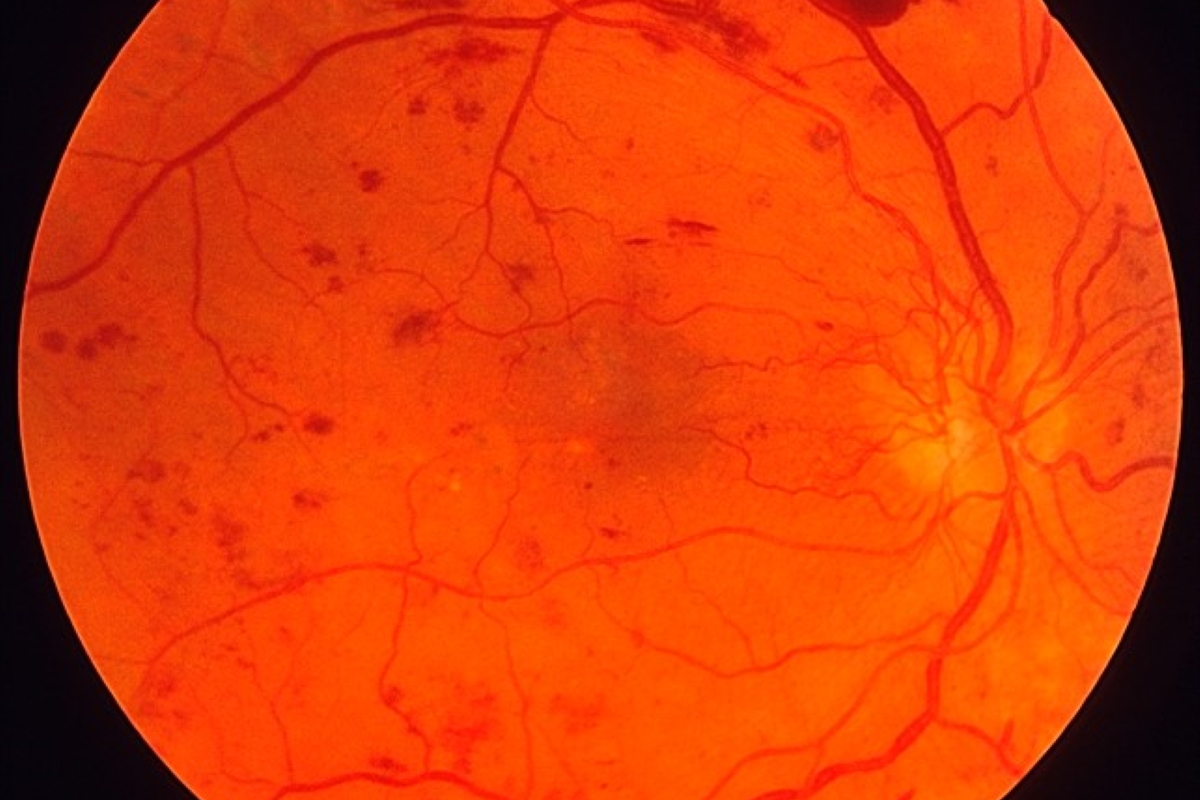
This is a serious stage of diabetic retinopathy and can lead to blindness if untreated. At this stage, New Blood Vessels form on the retina or at the optic disc. These vessels are fragile and are prone to bleeding on the retina and into the vitreous resulting in floaters and visual loss. If left untreated, there retina gets damaged resulting in irreversible visual loss and ultimately blindness.
3. Diabetic Maculopathy or Diabetic Macula Oedema
Diabetic maculopathy occurs when the leakage and swelling occurs at retina area at the centre of the eye called the macula causing blurring of vision. This is the most sensitive part of the eye responsible for fine vision and reading. If left untreated, the macula gets damages resulting in loss of central vision.
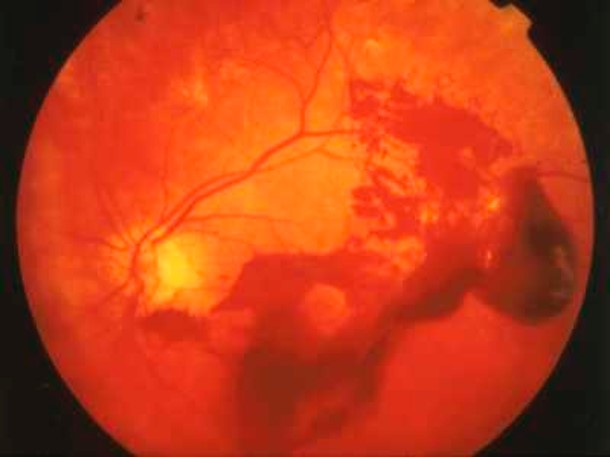
Image of Retina & Vitreous Haemorrhage
Treatment of Diabetic Retinopathy (DR)
Treatment depends of the type and severity of the eye disease. Your eye doctor may use one or a combination of the following treatment options;
1. Argon / Diode Laser Treatment treats diabetic retinopathy in 2 ways;
- It reduces retina swelling or leakage by sealing off the microaneurysms
- It slows the growth of new blood vessels in the eye
2. Intravitreal Anti-VEGF Injection blocks VEGF protein in the eye, thereby slowing the growth of new blood vessels in the eye. This will slow and stop the damage caused by these abnormal leaky blood vessels
3. Surgery using Vitrectomy and/or Laser and/or Intravitreal Injection. Vitrectomy procedure removes the blockage caused by the haemorrhage of blood from the leaky new vessels. During the surgery, the eye doctor may apply Laser as well as Intravitreal anti-VEGF injection to prevent further bleeding.
Prognosis for Diabetic Retinopathy
The visual recovery varies from person to person. The earlier the condition is treated, the better the outcome. Even after treatment, you still need to take good care and follow these recommendations because diabetic retinopathy can recur anytime throughout your life
- Check your own vision regularly (around 1-2 times a week) with a Vision Chart to detect early signs of any vision loss
- Check your own fasting blood glucose regularly (around 1-2 times a week or depending on your diabetic doctor’s recommendation) and document it on a notebook or on our Health Tracker feature on TELEME mobile app to share with both your diabetic doctor and eye doctor
- Have a blood test at a Lab Centre every 3 months to check on your HbA1c as well as other blood parameters such as kidney and lipid profile
- Get your eyes checked by an eye doctor every 4-12 months (or sooner if your diabetic control is not optimum). This allows any diabetic eye disease to be detected and treated early.
Remember that diabetes does NOT necessarily lead to visual loss. The good news is that you can take an active role in managing your diabetic control with your doctor to prevent any diabetic eye complications. Do click below to find an eye doctor near you to have an eye examination.
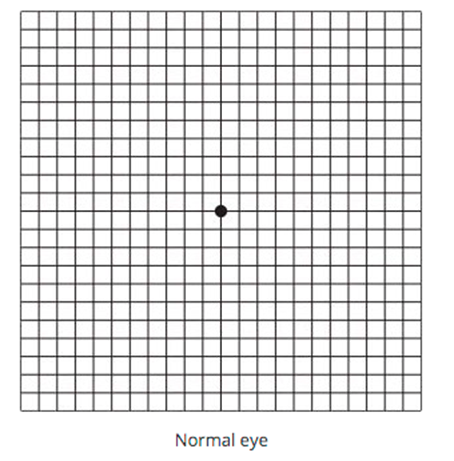
Check your vision regularly (at least once a week) using Amsler Grid and Vision Chart to monitor your condition

Disclaimer. TELEME blog posts contains general information about health conditions and treatments. It is not intended to be a substitute for professional medical advice, diagnosis or treatment. The information is not advice and should not be treated as such.
If you think you may be suffering from any medical condition, you should seek immediate medical attention from your doctor or other professional healthcare providers. You should never delay seeking medical advice, disregard medical advice, or discontinue medical treatment because of information on this website.