POLYCYSTIC OVARIAN SYNDROME AND FERTILITY SERIES PART 2
In PCOS and Fertility Series Part 1, you have learned about what is PCOS and how you get to know if you have PCOS. In this part 2 series, we will continue with how PCOS can affect your health.
General Health Consequences
PCOS can lead to general health condition known as metabolic syndrome. Metabolic syndrome consist of a cluster of problems, namely high blood pressure, high blood sugar level, increased fat around the waist and increased body cholesterol level. This occurs because PCOS leads to insulin resistance.
Insulin resistance is a condition where the body does not respond appropriately to a given level of body insulin. Insulin in a natural body hormone, produced by the pancreas, that regulates metabolism in our body. Insulin regulates sugar level by controlling the intake of sugar into our muscle and fat cells and also production of sugar from the liver. Hence, in PCOS, the body cells does not respond to insulin as they should be. This leads to sugar not being utilised by muscle and fat cells properly and it also increases production of sugar by the liver. This leads to increased sugar level in our body. Insulin resistance also leads to increased fat release into our circulation from fat cells.

This phenomenon of insulin resistance puts a woman at increased risk of developing Type 2 Diabetes Mellitus, increased blood pressure and high cholesterol. The combination of all this will finally increase the risk of heart disease.
Significant number of women with PCOS are overweight and obese. The usual complaint is they are putting on weight even with a careful and strict diet. This is related to insulin resistance and a high level of circulating insulin in the body. High insulin level is associated with weight gain in a woman with PCOS. So now you know that it’s not entirely your fault for not losing weight, its the insulin!

Fertility and Reproductive Health
In PCOS, the women often misses her periods. Do you know why ?
First of all , you need to understand the basic hormonal mechanism of your menses (period). In a typical 28-days period cycle, a woman’s egg (1 egg each period cycle) takes about 14 days to develop and released (ovulate) by Day 14 of the cycle (Day 1 is the first day of menstrual flow). During egg development, the capsule of the egg releases hormones that starts to thicken the lining of the uterus. After ovulation, the left over capsule of an egg further produces hormones that thickness the lining of the uterus to its maximum. If there is no fertilisation of the egg ( that means the man’s sperm did not enter the egg), the woman typical sees her period 14 days from ovulation (ie Day 28 from her first day of menses). The duration of the second half of the period (ie after ovulation), is quite constant.
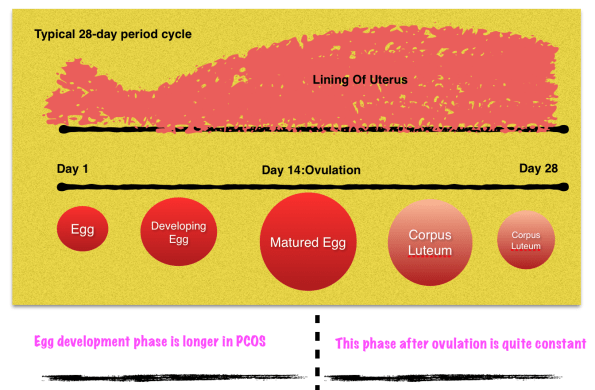
In PCOS, more often than not, the duration of egg development is quite long. It takes more than usual 14 days to develop. For example, if the egg takes 20 days to develop and ovulate, the woman will typically see her period on Day 34 of her cycle ( 20 days + 14 days= 34 days). A significant number of women do not ovulate at all for many months and they typically see only a few periods a year or not at all.
So, women with PCOS typically present with long period cycles or no period at all and their main complaint would be inability to get pregnant. This is due to lack of ovulation.
However, not all women with PCOS have problem conceiving. Some do get pregnant naturally with ease. So problem solved? Hold your horses, PCOS increases certain risk even in pregnancy.

The most important risk is Diabetes in pregnancy or known a Gestational Diabetes Mellitus (GDM). Remember about insulin resistance ? This phenomenon does not disappear once you get pregnant, in fact it continues. Insulin resistance can worsen and give rise to GDM.
GDM has a few unwanted adverse effects in pregnancy. It can lead to ‘big baby’ (macrosomia) with associated birth complications, preterm labour and intra-uterine fetal death.
The woman also faces increased risk of miscarriage in pregnancy. Research has shown that miscarriage rates in women with PCOS is about 2-fold higher. Some data also suggest miscarriage rate between 30-50% for women with PCOS undergoing fertility treatment.
The reason for increased risk of miscarriage could be a combination of insulin resistance, obesity and Diabetes in pregnancy.
Risk of Cancer
Another important consequences of PCOS which is least spoken about is risk of developing womb cancer (endometrial cancer).
In a women with PCOS who sees very few periods in a year or in whom there is no periods, the lining of uterus (endometrium) is often very thick. This is due to a combination of prolonged development of egg which prolonged the hormonal exposure of the uterine lining and no periods (which means no shedding of the thickened uterine lining).
Generally, women are advised to have periods at least once in 3-4 months. A very thick uterine lining if left for a long time, can cause the cell in the uterine lining to change into what the doctor’s call ‘hyperplasia’. Hyperplasia means increased rate of reproduction of cells. This is can lead to development of cancer if left unchecked for too long.
Since you now know the consequences of PCOS, you may be wondering if there is any way you can cure PCOS. Unfortunately, there is no cure for PCOS. However, you can treat PCOS with lifestyle changes and medical management and that’s what you will learn in Part 3 Series: “What can I do to help myself?”
Sources: NHS, MedicineNet, American Diabetes Association, American Cancer Society
Disclaimer. TELEME blog posts contains general information about health conditions and treatments. It is not intended to be a substitute for professional medical advice, diagnosis or treatment. The information is not advice and should not be treated as such.
If you think you may be suffering from any medical condition, you should seek immediate medical attention from your doctor or other professional healthcare providers. You should never delay seeking medical advice, disregard medical advice, or discontinue medical treatment because of information on this website.