Psoriatic Arthritis
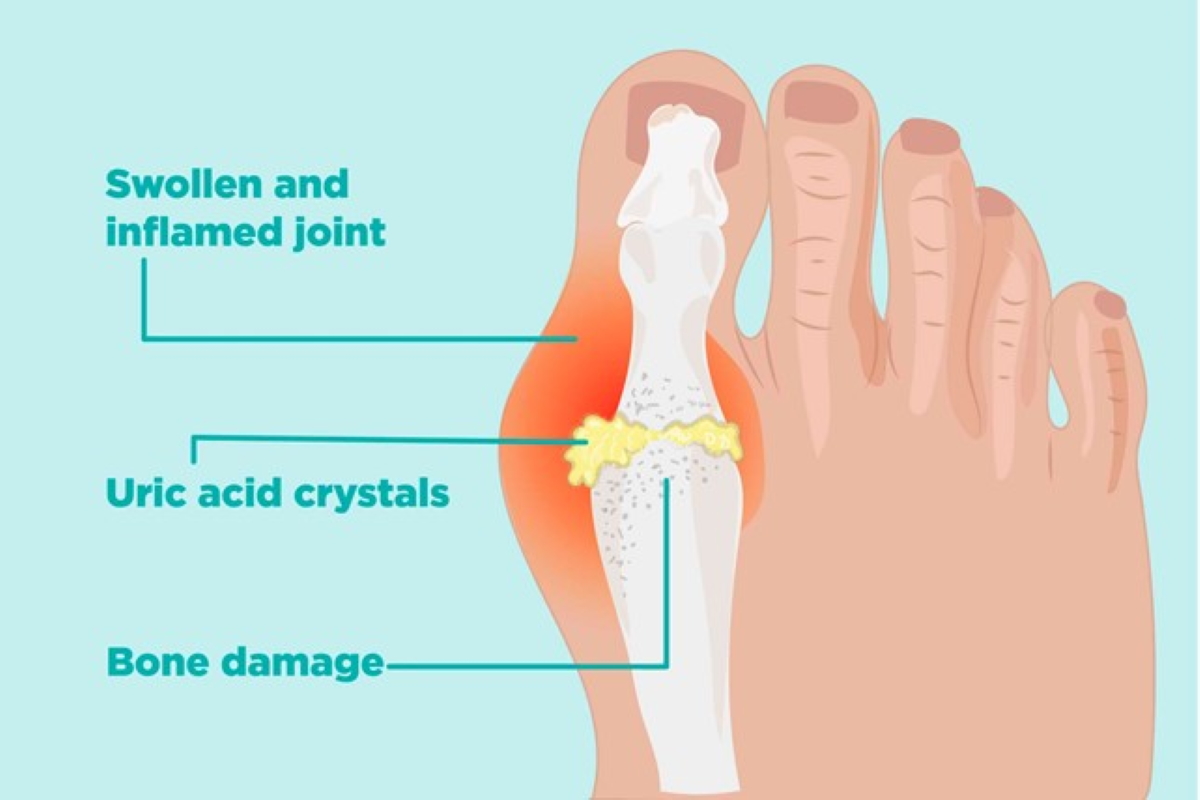
Psoriatic Arthritis is a chronic joint and skin disease due to auto-immune inflammatory disorder. It is often found in association with the skin disease Psoriasis (where there are scaly red and white skin patches on the body). It usually starts around the ages of 30-50 but can also affect children.
Symptoms
- Tiredness or fatigue
- Usually affects large joints like the knee and ankle
- Can also affect hands, wrists, fingers, pelvis and spine
- Fingers can be swollen and stiff
- The finger or toenails become pitted
- Sometimes the eye can get inflamed (known as uveitis)
Click to view John Hopkins Rheumatology video on Psoriatic Arthritis Treatment
Treatment
Treatment focuses on reducing inflammation to ease pain and stiffness as well as protecting the joint from permanent damage. Treatment will be tailored depending on the symptoms and severity of your disease.
Choice of medications
A. Analgesics (to help control pain)
Paracetamol, co-dyramol or co-codamol
B. Non-Steroid Anti-Inflammatory Drugs (NSAID) (to help control pain and reduce inflammation)
Aspirin, Ibuprofen, Nurofen, Meloxicam
C. Steroids (to reduce inflammation)
Prednisolone, Hydroxycortisone
D. Disease Modifying Anti-Rheumatic Drugs (DMARD) (to reduce immune system attack)
Methotrexate, Sulphasalazine, Leflunomide (Arava), Hydroxychloroquine
E. Biologics (to reduce the immune system attack by targeting specific immune cells)
Influximab (Remicade), Etanercept (Enbrel), Adalimumab (Humira), Certolizumab (Cimzia), Golimumab (Simponi), Tocilizumab (Actemra), Sarilumab, Rituximab (Rituxan), Abatacept (Orencia)
F. JAK Inhibitors (to reduce immune system attack by targeting specific proteins inside cells)
Tofacitinib (Xeljanz), Baracitinib (Olumiant), Upadacitinab (Rinvoq)
Monitoring Your Arthritis
Your doctor will use DMARDs as first line treatment for reduce the active inflammatory process so that your joints can be protected from permanent damage. As these medications take time to start working, you may need a combination of medication to include Steroids or NSAID which start working faster.
It is VERY IMPORTANT that you adhere to your doctor’s instructions because every patient will have different combinations of medication because of the varying degrees of disease presentation and tolerance to the side effects.
As your disease may fluctuate from time to time, it is also NORMAL for your doctor to change the strength of the medication or change the combination of your medicine.
Although it can be depressing to feel that your arthritis cannot are cured, be reassured that most disease can be controlled with medication. Remember that once your joints are damaged, the damage is permanent and irreversible.
Self Help and Monitoring
- Eat well and keep a healthy weight (biologics work better in people who are not overweight)
- Do gentle exercises to improve the joint mobility
- Regular physiotherapy can help to reduce your joint stiffness
- Do regular blood tests to monitor your blood counts, liver and kidney function due to possible side effects from the medication
- See your doctor if your symptoms suddenly get worse because you may have a disease flare-up or medication side effects
Remember to keep your follow-up appointments and do your blood tests regularly to help keep your disease in remission
Disclaimer. TELEME blog posts contains general information about health conditions and treatments. It is not intended to be a substitute for professional medical advice, diagnosis or treatment. The information is not advice and should not be treated as such.
If you think you may be suffering from any medical condition, you should seek immediate medical attention from your doctor or other professional healthcare providers. You should never delay seeking medical advice, disregard medical advice, or discontinue medical treatment because of information on this website.