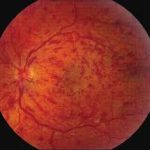
Keratoconus
Keratoconus occurs when your cornea becomes thinner and changes shape from being a regular round to an irregular cone or oval shape. This irregular shape makes the vision ‘fuzzy-like’ or double-imaged and becomes difficult for the optician / optometrist to measure to make spectacles or fit contact lenses.

Causes
There is no known cause for keratoconus but there appears to be a genetic predisposition because around 1 out of 10 people have a family history of keratoconus. The condition is more common in people with;
- connective tissue disease such as Marfan syndrome and Ehlers-Danlos syndrome
- excessive eye rubbing
- skin or eye allergy
- Down’s syndrome
Click to view Wills Eye Hospital video on Keratoconus
Symptoms
Keratoconus usually starts during teenage and slowly progresses for 10 to 20 years before it stabilises around the age of 30-40. Keratoconus affects both eyes although it usually affects one eye more than the other. The rate of deterioration varies between individuals with some progressing rapidly while others remaining stable for years.
- Gradual blurring or distortion of vision
- Frequent change in spectacle prescription
- Difficulty wearing contact lenses
- Sensitivity to bright light and glare especially at night
- Sudden worsening of vision to due scarring or oedema (known as hydrops cornea)
Diagnosis
A eye examination by your eye doctor with a corneal topography scan will be able to diagnose the condition. The scan shows typical corneal irregular astigmatism and corneal thinning.

Treatment
1. Spectacles or Rigid Gas Permeable Contact lenses may be able to improve the vision if the keratoconus is at a mild or early stage and the astigmatism is not too high or too irregular
2. Corneal Collagen Cross-Linking may help to slow down or stop the keratoconus from progressing and possibly prevent the need for a cornea transplant in future
3. Corneal Transplant may be required in severe cases when the cornea is extremely thin, has scarring or high astigmatism which cannot be corrected with glasses or contact lenses
Follow up
Have regular follow-up eye examinations with your eye doctor to monitor the progression of the keratoconus. It is important to detect any deterioration early and have treatment quickly so that the keratoconus does NOT progress to cause irreversible scarring.
Discuss your Treatment Options for your corneal condition with a Corneal Eye Specialist
Disclaimer. TELEME blog posts contains general information about health conditions and treatments. It is not intended to be a substitute for professional medical advice, diagnosis or treatment. The information is not advice and should not be treated as such.
If you think you may be suffering from any medical condition, you should seek immediate medical attention from your doctor or other professional healthcare providers. You should never delay seeking medical advice, disregard medical advice, or discontinue medical treatment because of information on this website.