Asthma Action (Treatment) Plan
An Asthma Action Plan (or Treatment Plan) is created by your doctor to help asthmatic patients like you to control your asthma effectively. Each plan may differ from patient to patient depending on the severity and condition of the disease. The plan may get reviewed and modified from time to time depending on how well the asthma is controlled.
The plan should describe (1) how and when to take your daily medications, and also (2) what to do during an asthmatic attack. If it’s your child who has asthma, all his/her caregivers such as teachers or sports coaches should be informed of the diagnosis.
As a patient, you also need to take an active role to control your asthma. This involves:
- Avoiding things that worsen your asthma (asthma triggers)
- Be aware of your environment such as air pollution (wear a mask or avoid going out) or weather changes (wear appropriate clothing)
- Understand your medication and never skip them. Always have access to quick-relief medication (especially when travelling)
- Learn to recognise the early symptoms of an asthma attack and take appropriate action
- Self-monitor to track your asthma using a peak flow meter on a regular basis and share these records with your doctor. You should also record your symptoms to discuss with your doctor at the next clinic visit
What is in the Asthma Action Plan?
Each Asthma Action Plan should give you the following information”
- The name of the medicines and how & when to take them
- How much medication to take in different circumstances
- When to take rescue medication
- How to use and chart your peak flow reading
- How to recognise signs if your asthma is getting worse
- What to do during an asthma attack
Asthma medication is divided into either;
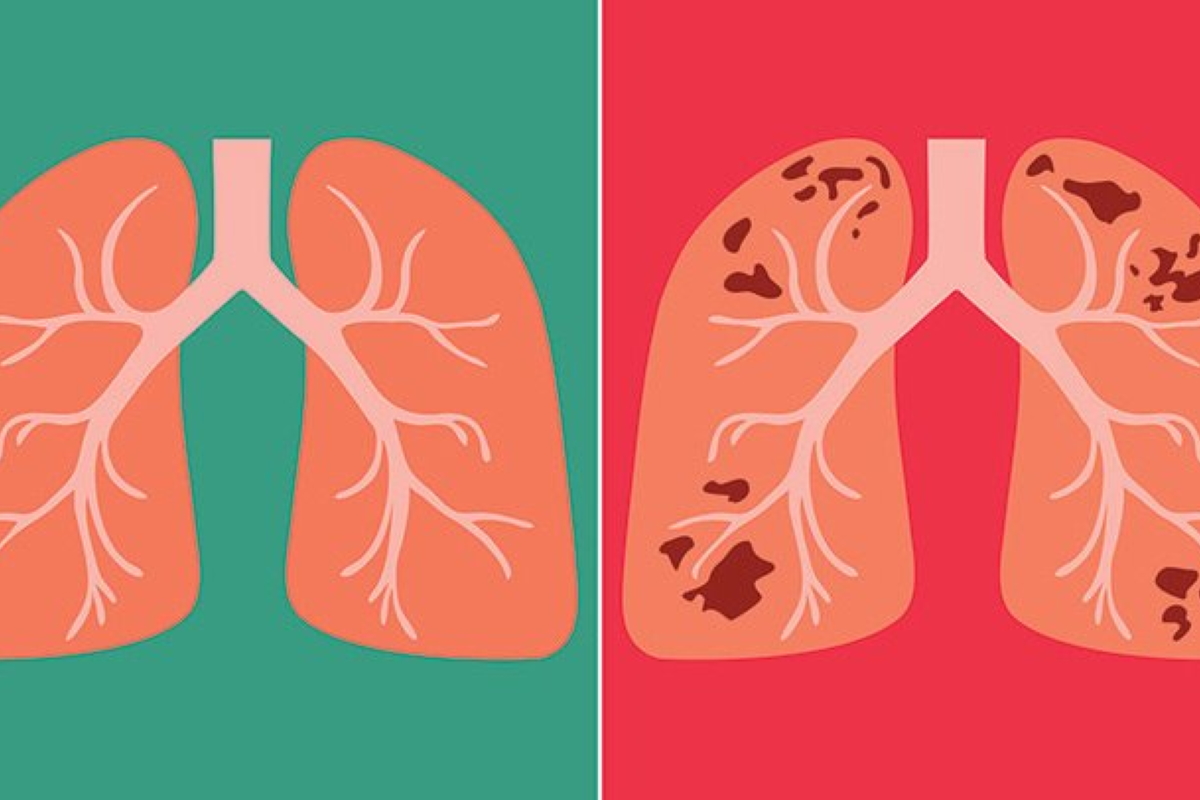
- PREVENTER inhaler (to reduce airway inflammation)
- RELIEVER inhaler (to open up the airways in the lung)
Simple Guide on How to Use the Asthma Medication
This guide shows how asthma medication may be used in different situations and in different individuals. Do consult your doctor about your own (or your child’s) situation.
Situation 1 (GREEN ZONE): When your (or your child’s) asthma is well-controlled
- Has good breathing
- Has no cough
- Has no wheezing
- Can play and do daily activities without any restriction
- Peak flow reading is more than 80% of personal best
ACTION PLAN: Use Preventer Medicine as prescribed by the doctor.
Situation 2 (YELLOW ZONE): When your (or your child’s) asthma is NOT well-controlled (with these symptoms)
- Cough or Wheeze
- Chest tightness
- Waking up at night due to coughing
- Peak flow reading is reduced to 50-80% of personal best
ACTION PLAN: Continue using Preventer Medicine as prescribed by the doctor. Use Reliever Medication as when required. You (or your child) may need up to 4 hourly medication depending on whether there is an improvement. If symptoms improve, return to Situation 1.
Situation 3 (RED ZONE): When your (or your child’s) asthma is getting worse
- The cough and wheeze getting worse despite treatment
- Difficulty in breathing with flaring around the nostrils
- The reliever medications needed more frequently than every 4 hours
- Peak flow reading is less than 50% of personal best
ACTION PLAN: Continue using preventer medicine as prescribed by the doctor. Use the Reliever Medication every 4 hours (and an oral dose of Prednisolone) as prescribed by the doctor. See your doctor AS SOON AS POSSIBLE.
Situation 4 (EMERGENCY): What to do during an during a Serious Asthma Attack
Take 4-6 puffs of reliever medication immediately and every 20 minutes up to a maximum dose of 12 puffs. Go IMMEDIATELY to the Emergency Department of the Nearest Hospital.
Disclaimer. TELEME blog posts contains general information about health conditions and treatments. It is not intended to be a substitute for professional medical advice, diagnosis or treatment. The information is not advice and should not be treated as such.
If you think you may be suffering from any medical condition, you should seek immediate medical attention from your doctor or other professional healthcare providers. You should never delay seeking medical advice, disregard medical advice, or discontinue medical treatment because of information on this website.