Type 2 Diabetes Treatment and Medication
Treatment of Diabetes
Currently there is no known cure but the disease can be controlled to enable the individual to have a better quality of life. The main aim of management is directed at reducing complications and prevent premature death by keeping consistently good diabetic control.
All patients with diabetes should undergo lifestyle modification, which consists of dietary therapy and increased physical activity. Unfortunately, more than 80% of patients still find difficulty keeping good control.
The need for oral medications or insulin therapy depends on the symptomatology, state of glucose control and the presence of any complications.
Target control for Type 2 Diabetes
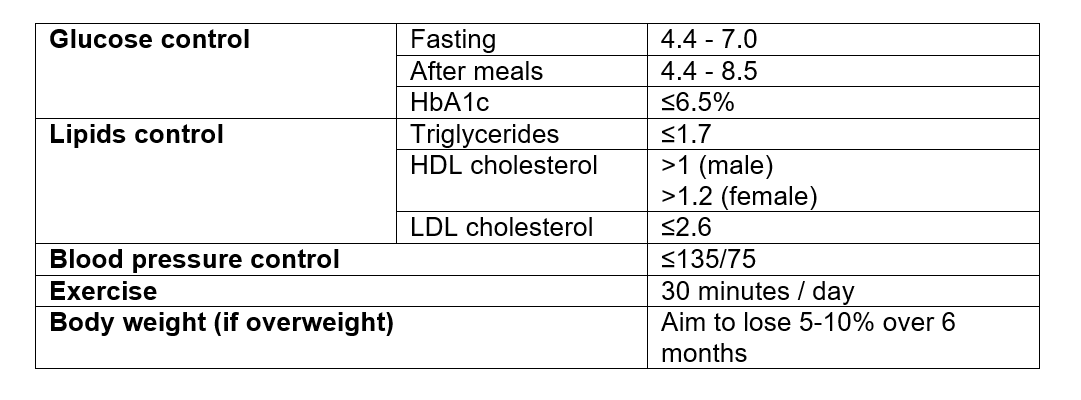
Choice of medication
If changing your lifestyle (such as diet, exercise or weight loss) has not improved your condition, your doctor may need to start you on medication. Oral Anti-Diabetic medication can be used as monotherapy or in combination with other OAD(s) and/or injectable agents such as insulin or GLP-1 receptor agonists.
1. Biguanides (Metformin)
Metformin lowers blood glucose especially fasting blood glucose by decreasing hepatic glucose production. It reduces HbA1c by about 1.5%. Most common adverse effects are nausea, anorexia and diarrhoea and can be minimised if it is taken together with/or after meal or taking the extended release (SR or XR) formulation.

2. Sulphonylureas
Sulphonylureas reduce plasma glucose by increasing insulin secretion. It reduces HbA1c by about 0.4-1.6%. It should be taken 30 minutes before meals. The major adverse effect is hypoglycaemia (this risk is higher in renal impairment, liver cirrhosis and the elderly) and weight gain. Be careful of drug interaction with NSAIDs, anti-thyroid medication and anticoagulants.

3. Meglitinides
Meglitinides also increase insulin secretion but bind to a different site within the SU receptor. It can reduce HbA1c by 1-1.2%. It should be taken 10 minutes before meals and is associated with less risk of weight gain compared to sulphonylureas and hypoglycaemia may be less frequent.

4. Alpha-Glucosidase Inhibitors (Acarbose)
Acarbose reduces the rate of absorption of polysaccharides in the small intestine by inhibiting glucosidase enzymes and should be taken with meals. It lowers postprandial glucose without causing hypoglycaemia but is less effective in lowering glycaemia than metformin or SU, reducing HbA1c by 0.5–0.8%. The side effects are bloating, abdominal discomfort, diarrhoea and flatulence.

5. Thiazolidinediones (TZDs)
Thiazolidinediones are peroxisome proliferator-activated receptor-gamma (PPAR-) agonists and act by increasing insulin sensitivity in muscle, adipose tissue and liver.
It can reduce HbA1c by 0.5–1.4% but improvement in glycaemic control may only be seen after six weeks with maximum effect at six months.
Side effects include weight gain (due to redistribution of body fat), fluid retention, heart failure, macular oedema and osteoporosis. They are contraindicated in patients with heart or liver failure.

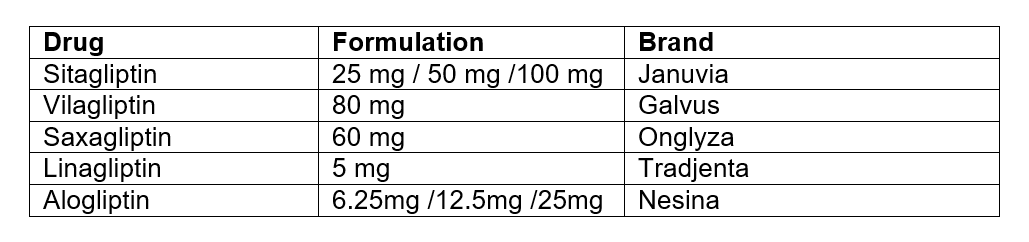
6. Dipeptidyl Peptidase-4 (DPP-4) Inhibitors
It lowers A1c by 0.5–0.8% and does not cause weight gain with minimal risk of hypoglycaemia.

7. Sodium-glucose Co–transporter 2 (SGLT2) Inhibitors
This class of drugs selectively inhibits SGLT2, a transporter in the proximal tubule, thus reducing glucose reabsorption leading to an increase in urinary glucose excretion. It reduces HbA1c by 0.2% to 0.8%. It is accompanied by weight loss (2.5 to 3.0 kg) and modest blood pressure reduction together with lower risk of hypoglycaemia. Side effects include significant increase of genitalia and urinary tract infection. It is not recommended in patients with kidney problems.

8. Insulin Injections
Insulin may be required when good glucose control cannot be achieved despite optimal OAD treatment. Sometimes, insulin may be required for short term use during pregnancy, acute illness or undergoing surgery. The ideal insulin regimen should mimic the physiological insulin response to meals and endogenous hepatic glucose production. The choice of insulin regimen is individualised by your doctor, based on your glycaemic profile, dietary pattern and lifestyle.
It is vital to perform Self-Monitoring Blood Glucose while on insulin especially when travelling on holiday because meal times may be different from your usual routine.

9. GLP 1 Receptor Agonist
This group of injectable medication mimics the function of natural Incretin hormone in your body that helps lower both post meal and fasting blood glucose by stimulating the release of Insulin from the pancreas. At the same time, it also inhibits the release of Glucagon during the fed state. It can slow the speed of stomach emptying after meals (thus making one feel more satisfied after a small meal) while increasing the feeling of fullness.
The effects are in response to the presence of food in the gut and therefore reduces the chance of hypoglycaemia occurring. It may help with weight reduction (between 4-6 kg of weight loss) and reduce the HbA1c by 1.5% while protecting the heart and kidney.
Side effects include nausea, vomiting, headaches, dizziness, diarrhoea, constipation, feeling of indigestion, loss of appetite and sweating.
| Drug | Brand |
| Exenatide | Bydureon, Byetta |
| Lixisenatide | Lyxumia |
| Dulaglutide | Trulicity |
| Liraglutide | Victoria |
Complications
Untreated diabetes can cause serious health problems in the long term such as:
- Heart disease and stroke
- Peripheral neuropathy
- Diabetic retinopathy
- Kidney disease
- Foot numbness or ulcers
- Sexual dysfunction
- Miscarriage
Discuss with your doctor or endocrinologist about your treatment options
Sources:1) https://www.niddk.nih.gov2) MOH Clinical Practice Guidelines on Management of Type 2 Diabetes 2015
Disclaimer. TELEME blog posts contains general information about health conditions and treatments. It is not intended to be a substitute for professional medical advice, diagnosis or treatment. The information is not advice and should not be treated as such.
If you think you may be suffering from any medical condition, you should seek immediate medical attention from your doctor or other professional healthcare providers. You should never delay seeking medical advice, disregard medical advice, or discontinue medical treatment because of information on this website.